- Fertility Treatments
- Fertility Preservation
- Donor Program
- Options For Same Sex Couples
- Options For Single Women
- Patient Support Services
Blastocyst Culture | What It Is & The Benefits
What is a blastocyst?
The term ‘blastocyst’ refers to the human embryo 5 - 6 days after fertilisation.
It is the stage of development that the embryo must reach before it can implant in the uterus.
The structure of the blastocyst is more complex than earlier embryo stages because as well as increasing in cell number, the cells have become organised into 2 types, the trophectoderm, whose main role is in the implantation into the uterine lining and the inner cell mass which will give rise to the foetus itself.
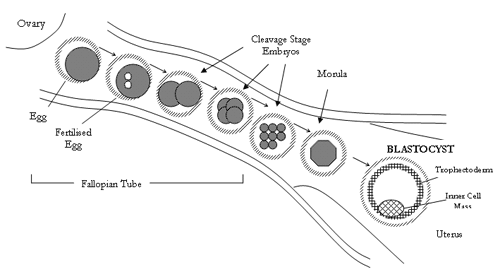
The diagram below shows blastocyst formation in the female body.
The egg is fertilised following ovulation from the ovary and the embryo goes on to divide (cleave) as it travels along the fallopian tube. Blastocyst formation occurs as the embryo reaches the uterus.
What’s so special about blastocyst culture in an IVF setting?
Standard practice in IVF involves the replacement of embryos into the uterus after 5 or 6 days when the embryos are at the blastocyst stage of development.
Why extend the time that the embryos are cultured in the laboratory?
It is known that a lot of embryos are destined to arrest at early stages so extended culture allows the embryologist to identify which (if any) of a group of embryos have the best potential for implantation by identifying those which form a normal blastocyst in culture.
Transferring embryos at the blastocyst stage also provides a better co-ordination between the embryo and the uterus by putting the embryo back in the right place (the uterus) at the right time (blastocyst stage).
What are the benefits of blastocyst culture?
Overall, if you have a normal blastocyst for transfer on day 5, the chances of pregnancy are higher (in our hands) than if you have embryos transferred on day 3.
However the chances of having no embryos for transfer at all are also higher.
Who is blastocyst culture appropriate for?
If your previous IVF treatment did not work despite the fact that you had embryos for replacement on day 2 or 3, blastocyst culture should help us determine whether in fact your embryos develop beyond day 3 at all (even very good quality day 3 embryos may not form blastocysts) and if so, which of those embryos would be the best ones to transfer.
Are there any benefits in younger patients in whom IVF is likely to work anyway?
As blastocyst culture can help to determine which embryos have the best chance of being able to implant, we can potentially reduce the number of embryos that we replace into the uterus and thereby reduce the risk of a multiple pregnancy. In women under 35 (without female factor infertility) we can therefore offer single embryo transfer and significantly reduce the risk of both twins and higher order multiple pregnancy (triplets and quads).
Is there any benefit for patients over 37?
Yes. We can avoid the need to transfer 3 embryos on day 3, by transferring 2 blastocysts on day 5. The small risk of triplets can be minimised without affecting the pregnancy rate.
What are the results of blastocyst culture?
In 2003, we carried out 76 blastocyst cycles in patients with previous multiple failed IVF cycles. 78% of those couples had blastocysts for transfer. 42% of those patients achieved an ongoing pregnancy. Blastocyst culture has become a very valuable tool in our treatment armoury.
However:
- The extra culture time required adds to both the financial and emotional cost of treatment– many couples find the wait over this period very difficult.
- It is possible that you may not have an embryo transfer at all – about 20% of the patients we have treated to date with blastocyst culture have not reached embryo transfer.
- It is less likely that there will be ‘spare’ embryos available for freezing.
- There is a slightly increased risk of identical twins reported in the literature associated with blastocyst culture.
To find out more about blastocyst culture please book an appointment with a fertility specialist or contact us.
